DeMyer historic and mostly classified into three types of holoprosencephaly (less severe to more severe) [6]:
- Holoprosencephaly Alobar
- Holoprosencephaly semilobar
- Lobar holoprosencephaly
In alobar holoprosencephaly (shown in the picture below), a loss of midline forebrain division resulting hemispheres monoventricle and participation.
Fluid attenuated inversion recovery coronal fluid attenuated inversion recovery magnetCoronal MRI image showing holoprosencephaly alobar.
Semilobar holoprosencephaly is characterized by incomplete division of the brain, resulting in partial separation of the hemispheres, usually back.
In lobar holoprosencephaly (seen in the image below), there is complete ventricular separation, with focal areas of incomplete cortical division or anterior falcine hypoplasia present.
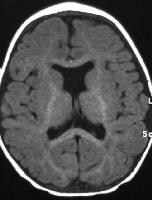
Axial T1-weighted magnetic resonance image shows septo-optic dysplasia, representing a variant of lobar holoprosencephaly.
Distinctive midline facial malformations occur in most cases. Typical facial anomalies are correlated with the degree of holoprosencephaly and have prognostic importance.[1, 2] From most severe to least severe, these include the following: (1) cyclopia, in which a single, midline, fused eye exists in a single orbit below a proboscis; (2) ethmocephaly, in which ocular hypotelorism is present with an interorbital proboscis; (3) cebocephaly, in which ocular hypotelorism is present with a single-nostril nose; (4) ocular hypotelorism and midline clefting; and (5) ocular hypotelorism and bilateral clefting.
More subtle facial dysmorphic features may also be present. These include a flat nasal bridge and tip; a single, midline, upper incisor; a bifid uvula; absent nasal bones and nasal septum; and congenital nasal pyriform aperture stenosis (decreased width of the nasal pyriform aperture at the level of the interior meatus).
Microcephaly is the rule, and macrocephaly, if present, is suggestive of hydrocephalus.
Virtually all surviving individuals with the more severe forms of holoprosencephaly have some developmental delay, often persisting as mental retardation. In general, this finding is directly correlated with the severity of holoprosencephaly.
Also not uncommon are seizures, hypotonia and/or hypertonia, extrapyramidal features, such as dystonia and/or chorea; hypothalamic and brainstem dysfunction leading to autonomic dysfunction and swallowing difficulties; pituitary dysfunction, which can manifest as partial or complete panhypopituitarism with resultant endocrine deficiencies; and feeding difficulties, which can lead to aspiration pneumonia and failure to thrive.
Active research into the pathophysiology of holoprosencephaly has revealed multiple teratogenic and genetic causes (chromosomal and single gene); further genetic characterization is ongoing.
Preferred examination
The imaging study of choice for the diagnosis and classification of holoprosencephaly is cranial magnetic resonance imaging (MRI).[7, 8, 9] The next best imaging modalities are ultrasonography and cranial computed tomography (CT) scanning.[1, 2, 10, 11, 12] Ultrasonography can be limited in cases of microcephaly if there is a very small fontanelle. Transcranial ultrasonography, however, can be performed through the calvaria, at times using the thinner temporal bones. Often this technique requires a transducer of lower frequency, resulting in better penetration, albeit at the loss of some near-field resolution.Prenatal evaluation by means of transabdominal or transvaginal ultrasonography can be used to identify most cases of alobar or semilobar holoprosencephaly. Prenatal MRI can be done in cases in which the infant's head is not easily accessible at the time of ultrasonographic evaluation or in cases in which the anatomy is not satisfactorily delineated at prenatal ultrasonography.
Limitations of techniques
Prenatal ultrasonography is not a reliable method for diagnosing mild forms of holoprosencephaly, such as lobar holoprosencephaly, because of its high false-negative rate. In addition, prenatal ultrasonography often cannot distinguish between alobar holoprosencephaly and semilobar holoprosencephaly. A transabdominal ultrasonographic diagnosis of holoprosencephaly before 16 weeks' gestation is difficult.Source : http://emedicine.medscape.com/article/409265-overview#a01